Tens of thousands of COVID-19-positive patients were hospitalized in Northern California last year. It was physicians, nurses, respiratory therapists, and many more who were at their bedside, providing exceptional care. Today, hear from ICU staff.
Reflecting on 2020, a year that forever changed the world, “feels like a dream,” said Venice Laquian, RN, an ICU nurse at the Kaiser Permanente South San Francisco Medical Center.
“It’s surreal and unbelievable looking back,” said the mother of 2.
When COVID-19 patients first began being admitted to Kaiser Permanente Northern California ICUs last spring, it was a time of uncertainty. “Because it was a new virus, the medical community didn’t know how it was spread or treated,” Laquian said.
ICU staff quickly met the challenges of the unknown and worked tirelessly through multiple COVID-19 surges, which at times filled ICUs to capacity with patients often staying 30 or more days. Kaiser Permanente hospitals typically manage one ICU, but during the surges some were managing up to 3, according to Stephen Parodi, MD, associate executive director of The Permanente Medical Group and national infectious disease leader for Kaiser Permanente.
To help with staffing, many non-ICU employees with critical care backgrounds were transferred to ICUs with high volumes of patients. “Kaiser Permanente was able to operate as a 21-hospital system, as opposed to 21 individual hospitals,” Dr. Parodi said.
Michelle Gaskill-Hames, senior vice president of Hospitals and Health Plan Operations, said, “It was inspiring to witness our teams coming together across geographies, functions, and roles to support the collective mission of caring for each and every patient that needed our care.”
The surges were among the most challenging times, professionally and personally, for Laquian.
“I often would cry about my patients,” said Laquian, who had moved into an in-law unit at her parents’ house out of fear of infecting her family. “Because our patients couldn’t be with their families, we were their eyes and ears. When families asked how their loved ones were doing, I had to be truthful. It was difficult.”
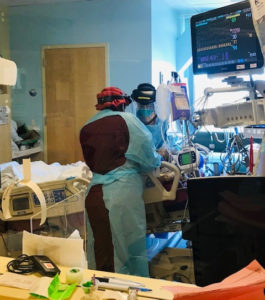
In communities with high-density, multigenerational housing, multiple members of the same family were often admitted with COVID-19. Gregory Marelich, MD, chair of Critical Care Medicine for Northern California and chief of Critical Care Medicine at the Kaiser Permanente South Sacramento Medical Center, told the story of a mother, father, and son who were battling the virus. The mother of the family did not survive.
“It’s not the physical laboring that has had lasting effects on us. It’s the emotional struggles that we all went through that we will remember.”
ICU adaptability saved lives
Though there is no cure for COVID-19, there has been progress in treating it. A point of pride for the Kaiser Permanente Northern California ICU teams were their ability to adapt to the rapidly changing protocols and patient care strategies.
“Our staff demonstrated extraordinary strength, resilience, and flexibility as they rose to address one challenge after another with steadfast resolve and courage,” said Gaskill-Hames.
ICU patients were initially treated with traditional methods of ventilation, but as knowledge for how to treat the virus grew, ICU staff adapted to the latest evidence using anti-viral and anti-inflammatory medications, high-flow oxygen, and proned (laid on their stomach) ventilation to achieve better outcomes, according to Dr. Parodi.
“Throughout the ever-evolving environment and the sheer volume of patients that ICU staff were caring for, they were always focused on the moment,” he said. “Something that never changed was the staff’s complete and utter resolve to do their best for their patients.”
“I have never seen so much suffering of people in my life and at the same time so much compassion.”
A greater appreciation for life
Yan Kim MD, a critical care physician at the Kaiser Permanente Santa Clara Medical Center, said last year showcased the unwavering bravery, resiliency, and dedication of her staff.
“It was the longest and hardest year of my and many of my colleagues’ careers,” she said. “I have never seen so much suffering in my life and at the same time so much compassion.”
A sentiment shared among all the ICU employees interviewed was their greater appreciation for life after the pandemic. The compassion shown to health care workers by people everywhere was what kept them going, Dr. Kim said.
“The kindness and generosity of people in our community is something that brought hope into this world of darkness.”




This Post Has One Comment
I am speechless and no words can describe the gratitude that I would like to express to all the staff that took care of my mom and all the love and the communication that keep us to date while my mom was in Kaiser San Leandro suffering from Covid-19. In our prayers we asked for my mom to have some angels taking care of her and that is what she had, angels in scrubs giving their lives to save the lives of others. All our love and prayers to Kaiser Permanente heroes and angels <3